Waxing lyrical
In OTC
Follow this topic
Bookmark
Record learning outcomes
Everyone has earwax, but for some people it can cause as many problems as it solves, especially if it becomes impacted. Understand how pharmacy teams can advise customers in preventing and managing this common condition
Visit a zoo and you’ll probably see a shed snakeskin pinned to the wall. People don’t slough their skin in one go like a snake, but, according to Imperial College London, a person loses almost five billion dead skin cells a day, which fall or rub off as they go about their everyday life. The skin continually makes new cells, so it is replaced approximately once every four weeks.
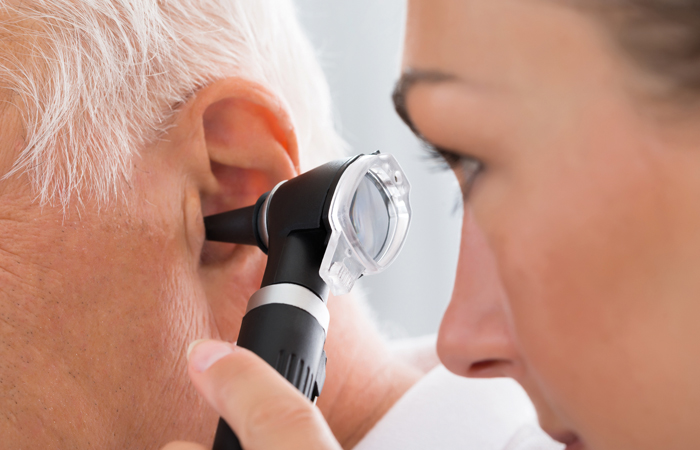
But the ear canal is a cul-de-sac – the only cul-de-sac of skin in the body – and dead cells can’t fall away as easily. Instead, they form part of earwax (cerumen). Usually, cerumen falls out of the ear without people noticing. But in some people it can block the ear canal, causing hearing loss, irritation and pain. So, what does a leading ear, nose and throat (ENT) consultant think pharmacy teams can help customers manage this common problem?
Introducing earwax
Earwax is a mix of dead skin cells, sebum – an oily substance that protects, lubricates and waterproofs the skin – sweat and other secretions. As earwax moves along the ear canal, aided by jaw movements, it cleans, protects and lubricates the skin. “Some studies suggest that earwax may reduce growth of some bacteria and fungi,” says Dr Nirmal Kumar, consultant ENT surgeon at Wrightington, Wigan and Leigh NHS Foundation Trust, and honorary professor at Edge Hill University Medical School. “But whether cerumen is an active, natural antibiotic is unclear. However, earwax probably acts as a physical barrier to infection.”
Earwax can build-up in people who produce too much, or when the self-cleaning mechanism does not work properly, both of which can cause what is known as impacted earwax. In 2007, some colleagues and I [Mark Greener] published a paper in the medical journal QJM, in which we provisionally estimated that between 1.2 million and 3.5 million people in the UK have impacted earwax. Of these, 2.3 million people experience problems serious enough to need management. These were best guesses – there is not a lot of evidence. Meanwhile, the growing population means that these figures have probably risen. But impacted earwax is clearly common and there is a lot that sufferers can do to help themselves.
Managing the problem
The first step is to ensure patients don’t have a more serious problem, such as an infection or a foreign object in their ear canal. “Diagnosing excessive earwax is straightforward: patients feel that their ears are blocked and they don’t have any other symptoms,” explains Dr Kumar, who is also president of ENT UK – the UK’s main professional body for ear, nose and throat specialists. “You can see the wax using an otoscope and the hearing loss develops suddenly. Typically, a patient may have most of their eardrum covered with wax, but they can still hear. But there’s a tipping point: the final bit of wax means that they can’t hear.” Dr Kumar suggests referring patients who feel generally unwell – those with a fever for example – and people with ear pain or other signs of an ear infection to their GP. Some may just have impacted earwax, but it’s best to be on the safe side.
Children are often unable to resist sticking objects in their nose and ears. “Objects in the nose need to be removed urgently to prevent inhalation,” Dr Kumar says. “Those in the ear need to be removed carefully by an ENT doctor using a microscope. Patients or parents shouldn’t try to remove the object – they could damage the ear or push the object deeper into the canal. So, while it needs to be removed as soon as possible, a foreign object in the ear doesn’t need a visit to A&E in the middle of the night. It can wait to morning.”
But there is an important exception: swallowing or inserting a button battery – such as those used in watches and hearing aids – is a medical emergency. Patients must go to A&E immediately. In 2014, NHS England warned that ingesting button batteries “can cause serious harm and death” from a build-up of sodium hydroxide (caustic soda). When swallowed, the sodium hydroxide burns tissues, such as in the oesophagus (food pipe). In some cases, the sodium hydroxide burns through blood vessels causing major bleeding. Symptoms of tissue damage, such as bleeding and breathing issues, can emerge up to 28 days after ingesting the battery. Even apparently flat batteries cause damage. Button batteries pushed into ears or nostrils can also, NHS England notes, cause serious injuries. “It’s essential to remove the battery from the ear, nose or gastrointestinal tract as soon as possible,” Dr Kumar says. “In addition, all patients need careful monitoring and follow-up.”
Between 1.2 million and 3.5 million people in the UK have impacted earwax
Removing earwax
Dr Kumar often suggests that people with excessive earwax put a couple of drops of warm – not hot or boiling – olive oil into their ears a couple of times a day, which softens and loosens impacted cerumen. Some patients may prefer over-the-counter ear drops. “There isn’t compelling evidence that any one product is better than any other,” he says. “However, the over-the-counter products seem to work more rapidly than olive oil.”
If olive oil or over-the-counter products don’t dislodge the cerumen, patients should see their GP, Dr Kumar advises. A doctor or nurse can remove earwax using a microscope, a strong light and precise suction. Some GP surgeries now offer this service. In other cases, patients might need to be referred to the local ENT clinic. Syringing, once the most common treatment, is becoming less popular. “We’re syringing fewer and fewer ears,” Dr Kumar says. “Although complications in people with normal ears are rare, syringing has occasionally burst the ear drum. Suction is more expensive, but it is more accurate and safer than syringing.”
Identifying the signs

Signs and symptoms of an ear infection that might warrant referral to a GP include:
- Difficultly hearing
- Discharge from the ear
- Feeling of pressure or fullness in the ear
- High temperature (38°C or above)
- Itching or irritation in and around the ear
- Lack of energy
- Pain in the ear
- Scaly skin in and around the ear
- Vomiting.
Additional symptoms in young children and babies include:
- Irritation and restlessness
- Keep losing balance
- Not eating as usual
- Not reacting to some sounds
- Rubbing or pulling the ear.
Chuck the candles, bin the bud
Pharmacy teams should advise against placing a lighted, hollow candle in the ear canal. According to the medical journal Canadian Family Physician, some alternative practitioners believe that burning an ear candle creates a vacuum that pulls earwax, debris and bacteria from the canal. Others suggest that the warmth of the candle melts earwax, which comes out of the ear over the next few days. But residue from the candle can fall into the ear and users might mistake the candle residue for dislodged earwax. Dr Kumar adds that there is no good, scientific evidence that ear candles work. Indeed, ear candles can cause burns, block the canal and produce temporary hearing loss. “Ear candles may dislodge earwax that is already loose,” Dr Kumar comments. “At best, however, ear candles are ineffective for impacted cerumen. At worst, they can occasionally lead to a perforated eardrum. We should advise against their use.”
Sticking cotton buds into the ear may seem harmless, but can cause injuries. “People should never put a cotton bud or any other item into their ear,” Dr Kumar says. “It’s a natural human tendency to want to clear or to poke something in the ear if it itches or feels blocked. But cotton buds and other instruments can push the wax further in and cause trauma, such as perforating the eardrum. It’s really dangerous.”
In 2017, research in the Journal of Pediatrics looked at 263,338 children with ear problems related to cotton buds who presented to emergency departments in the USA. A foreign body, such as bits of the bud (29.7 per cent), perforated eardrum (25.3 per cent) and tissue damage (23.1 per cent) were the most common injuries associated with cotton buds. Lacerations and cuts accounted for one in 20 (five per cent) injuries. About three-quarters (73.2 per cent) of injuries occurred during ear cleaning, while about one in 10 occurred during play (9.7 per cent) or following an accident, such as a fall or trip (9.3 per cent). Three-quarters of injuries (76.9 per cent) occurred when the child was handling the cotton bud. Use by parents and siblings accounted for the remaining injuries (15.8 per cent and 6.2 per cent respectively). “Cotton buds can cause immense damage to the ear,” Dr Kumar remarks. “Again, we should strongly advise against their use.”
Dr Kumar suggests that the only time anyone should let a cotton bud anywhere near their ear is to clean discharge from an infection or excess liquid after instilling ear drops. In these cases, a cotton bud can mop up the fluid. However, a cotton wool pad does just as well.
Impacted earwax is one of the most common problems pharmacy teams will encounter. After all, between one in 17 and one in 50 (two to six per cent) of the general population have impacted earwax. A build-up of earwax is even more common in some groups: about a third of those with intellectual disabilities and up to half of the elderly have impacted earwax, for example. Usually, pharmacy staff can reassure customers that there’s nothing to worry about. But tell them to chuck the candles and bin the buds. A few drops of warm olive oil or one of the preparations on the pharmacy’s shelves is all that’s usually needed to dislodge a build-up of wax, resolve the hearing loss and alleviate that unpleasant blocked feeling.
