Sound advice
In OTC
Follow this topic
Bookmark
Record learning outcomes
The ears can be affected by a diverse range of problems that can all impair hearing

Learning objectives
After reading this feature you should:
- Understand how to manage common ear complaints
- Be able to provide practical strategies for customers to safeguard their hearing
- Recognise the benefits of hearing aids and implants for those customers with hearing impairment.
With estimates indicating that around one in every six people in the UK currently suffer with hearing loss or deafness,1 pharmacies can play a key role in managing common ear complaints, advising customers on protection against noise-related hearing loss and helping to encourage the uptake and optimal use of hearing aids.
Earwax
Earwax or cerumen is a protective wax produced by tiny glands near the entrance to the ear canal. The function of earwax is to trap dust, dirt and microorganisms, helping to keep the ear canal clean and clear so sound can pass through easily. Earwax also provides a protective coating over the skin of the ear canal, which acts as a temporary water repellent. The ear itself is designed to be self-cleaning and wax usually works its way to the outside of the ear and falls out spontaneously, but sometimes it can accumulate inside the ear canal and cause problems.
Although easily dismissed as a minor ailment, earwax build-up is actually a leading cause of GP consultations for hearing impairment and can cause a range of symptoms including earache, a blocked feeling in the ear, itchiness, dizziness, tinnitus, and even cough. Figures suggest that 2.3 million people in the UK experience problems with earwax each year.2
Hearing aids and the regular use of earplugs can act to push wax further into the ear canal. Wax also becomes naturally harder with age, which can contribute to the problem. Customers should be cautioned never to put their fingers or objects like cotton buds into their ears in an attempt to clean them or remove wax, as this will push the wax further in, exacerbating the blockage and could also damage the delicate inside of the ear or even rupture the eardrum itself.
Most cases of earwax will respond to self-treatment with simple olive or almond oil drops applied into the ear twice daily for three days. A range of specific OTC products are also available to soften and dissolve the wax. Ear drops should be applied at room temperature to the affected ear(s).
Suggest that customers lie on their side for a few minutes after application (with the blocked ear facing upwards) to allow the drops of solution or oil to soak fully into the wax. With treatment, lumps of earwax should dislodge naturally from the ear and fall out (usually while sleeping) over the following week or so.
For more tenacious earwax that fails to respond to OTC treatment, ear irrigation or microsuction by a specialist may be required. There is no evidence to support the value of ear candles or ear vacuums for the treatment of excess wax.
Swimmer’s ear
Swimmer’s ear or otitis externa is a bacterial or fungal infection affecting the outer segment of the ear canal. It occurs when excess water enters the ear canal, stripping away the protective earwax coating and allowing germs to enter and thrive. Symptoms include pain, redness and itching in the ear, hearing difficulties (sounds may become muffled as the ear canal swells) and ear discharge. A key diagnostic clue for otitis externa is pain when the outer ear (the pinna) is pulled or pressed.
Oral antibiotics are rarely indicated for cases of localised otitis externa, with management centring on analgesics and the application of topical heat. Both paracetamol and ibuprofen can be recommended to relieve earache associated with otitis externa. Pressing a warm (but not wet) flannel against the infected ear may also help to reduce any pain.
For customers suffering with ear discharge, this can be removed by wiping the ear gently with cotton wool. Plugging the ears with cotton wool is not recommended. Ear drops or sprays containing acetic acid, which acts to block the growth of bacteria and fungi in the ear canal, can be used to treat mild cases of otitis externa.

In more severe cases, treatment with an antibiotic/antifungal or steroid ear drops or sprays may be required. Suggest customers visit their GP if the earache does not improve after three days, they have systemic symptoms such as fever and/or they have a concomitant long-term medical condition or a suppressed immune system. All sufferers of otitis externa should be advised to abstain from swimming or water sports for at least seven to 10 days.
According to NICE, the following self-care advice should also be provided to people with otitis externa to aid recovery and reduce the risk of future infection:3
- Prevent damage to the external ear canal by practising safe earwax removal and avoiding use of cotton buds or other objects for cleaning
- Ensure ears are kept clean and dry by using ear plugs and a tight fitting cap for swimming; drying the ear canal with a hairdryer on a low heat setting after hair washing, bathing or swimming; keeping shampoo, soap and water out of the ear as much as possible when showering or bathing
- Control dry skin conditions that are linked to the development of otitis externa – such as allergies/skin sensitivities and chronic skin complaints like eczema and psoriasis
- Consider the use of acidifying ear drops or sprays as a preventative measure before and after swimming.
Otitis media
Otitis media is an infection that occurs in the middle ear – deeper inside the ear canal than otitis externa. It is particularly common among children, of whom 80 per cent will suffer at least one middle ear infection before reaching the age of two years.4
The shape of the Eustachian tube in children tends to be shorter and more horizontal, which means fluid and mucus accumulate more readily in the middle ear. Bacteria can then travel up this fluid-filled Eustachian tube from the nose or throat to infect the middle ear, causing pain and inflammation.
Otitis media often strikes after a viral infection, such as a cold or flu, which causes the Eustachian tube to become blocked with fluid. The primary symptom is earache (young children may rub or tug their ears), which can also be accompanied by other non-specific symptoms such as fever, irritability, poor feeding, cough or runny nose.
To manage the pain of otitis media, pharmacy teams should recommended regular doses of paracetamol or ibuprofen, using a dosing schedule appropriate for the age and weight of the child. There is no evidence to support the use of decongestants or antihistamines to manage symptoms.
Given that otitis media is typically a self-limiting condition (three days to one week average duration), antibiotics are not routinely recommended. However, NICE does suggest antibiotic therapy for ear infections that fail to improve after three days if there is fluid or pus discharging from the ear or if the patient has co-morbidities that may predispose them to complications.
Antibiotics may also be prescribed for children under two years of age with a bilateral infection. Some GPs will opt to issue a ‘back-up’ antibiotic prescription for patients with otitis media – with advice to only fill the prescription if symptoms do not improve within three days or worsen rapidly.
As otitis media is usually triggered by a viral infection (e.g. a cold or flu, prevention of future occurrences is difficult. Parents should be advised to keep their child’s vaccinations up to date and avoid exposing them to second-hand smoke where possible. Using a dummy can also increase the chances of contracting an acute middle ear infection.
Key facts
- In the UK, around one in six people suffer with some degree of hearing loss or deafness
- Age and noise exposure are key factors leading to ear damage and the development of hearing loss
- Ear infections and problems such as excess earwax and glue ear can also contribute to hearing impairment.
Glue ear
Glue ear is a type of chronic otitis media that arises due to a build-up of thick or sticky fluid in the middle ear behind theear drum, causing temporary loss of hearing. This may be accompanied by earache/ear pain and ringing, buzzing or popping sounds akin to tinnitus.
Glue ear is surprisingly common – around eight in every 10 children will experience at least one episode by 10 years of age – but the condition usually resolves itself within a few months.4
For some children, however, glue ear poses a persistent, ongoing problem associated with long-term hearing impairment that can have a knock-on impact on education, language development and behaviour.
Parents may suspect glue ear if their child is mishearing, asking for words to be repeated, turning up the television, speaking loudly, not responding when spoken to (especially from behind) or becoming easily distracted/having difficulty concentrating.
Although no OTC treatment options for glue ear exist, reducing children’s exposure to second-hand smoke is a vital first step as this is directly linked to glue ear risk. Other factors that increase the likelihood of developing glue ear include repeated cold and throat infections, allergies and being bottle-fed while lying down.
When addressing a child with glue ear, it is important to speak slowly and clearly and ensure their attention is engaged before talking. Cutting down on background noise can also help with concentration and hearing. Reading with children every day is proven to develop their language skills and can help to overcome any negative impact of glue ear on education and learning.
Parents of a child with glue ear symptoms that have persisted for more than three months should be encouraged to consult their GP. The usual management approach involves monitoring for up to one year but autoinflation may also be carried out to open up the Eustachian tube and allow fluid to drain out. This technique involves the child closing their mouth and one nostril and then blowing up a small balloon using the other nostril.
There is no evidence for the efficacy of antibiotics, anti-histamines, steroids or decongestants in the treatment of glue ear so these should not be recommended. Customers should also be cautioned against use of complementary therapies or special diets as these remain unproven.
Hospital-administered treatment for intractable glue ear associated with significant hearing impairment include grommets and hearing aids. Grommets are thin plastic tubes inserted into the ear drum surgically (under general anaesthetic) that allow air to pass through the ear and fluid to drain out. They usually remain in place for six to 12 months before falling out naturally as the ear drum closes.
Noise-induced hearing loss
Exposure to loud noise currently ranks as the second leading cause of hearing loss after age-related deteriorative changes in the inner ear.1 Tinnitus can act as an early warning sign that hearing is being damaged by excess noise.
People may be exposed to excessive noise levels in the workplace or through their hobbies. Both sustained high-volume background noise and loud bursts of sound such as gunshots or explosions can damage the delicate structures within the ear.
To prevent noise-induced hearing loss, prolonged exposure to sounds louder than 85 decibels (dB) should be avoided. Above this threshold, sound-sensing hair cells in the cochlea start to sustain damage by becoming overstimulated and fatigued.
Although hair cells can recover from short episodes of excess noise, with sustained exposure they lose their ability to regenerate and start to die off – leading to noticeable and permanent hearing loss. As a rule of thumb, if a person standing two metres away cannot be heard without shouting, then the background noise level is likely to be hazardously high. To put this in perspective, just 15 minutes’ exposure to the average volume of nightclub music (100dB) is enough to increase the risk of hearing damage.

Practical advice
Fortunately, there are practical steps that pharmacy customers of all ages can take to help protect against noise-induced hearing loss. These include:
- Leaving the area or stopping the activity immediately if the noise generated is so loud it hurts the ears
- Using appropriate ear protection if exposed to unavoidable noise (e.g. at work). Employers are legally obliged to take action if noise exposure at work exceeds 80dB
- Using a volume limiter when listening to music and taking frequent breaks of at least five minutes to allow the ears to rest.
For customers who require ear protection, pharmacy staff can offer advice on choosing the equipment that best suits individual needs, such as earplugs, earmuffs and canal caps.
Attenuation describes the extent to which ear protectors reduce sound and is denoted in dB or a single simplified noise-level reduction (SNR) figure. Earplugs are generally preferred for long-term protective use and customers should choose a brand with a SNR of 20 or above that is specifically designed for hearing protection. Most industry-standard earplugs have a SNR of 25-32dB.1
Earplugs come in several different varieties including disposable/reusable types, custom-made products and specific earplugs for catering, shooting and music. Earmuffs and canal caps may be best suited to sporadic noise exposure as they can be easily taken on and off.
Hearing aids and implants
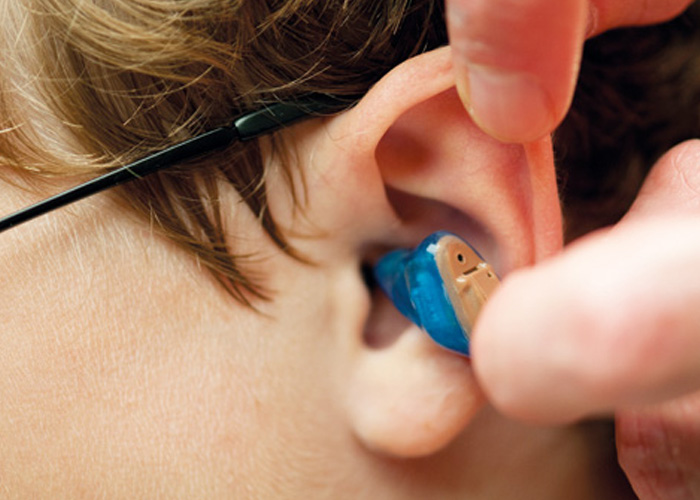
Hearing aids boost the volume and clarity of sounds, helping to reduce the impact of hearing loss on everyday lives. Those supplied by the NHS are typically behind-the-ear (BTE) devices, which deliver sound waves into the ear canal via either an ear mould that sits outside the ear or a small soft tip known as an ‘open ear fitting’.
Other hearing aid options include receiver-in-the-ear (RITE) or loudspeaker-in-the-ear BTEs that consist of a clear tube containing a wire that runs from the main body of the aid to a loudspeaker held in the ear by a soft ear piece.
Customers can often be reluctant to acknowledge hearing loss or consider the use of hearing aids, viewing the devices as a visible sign of disability and synonymous with old age. Pharmacy staff can help overcome this reticence by highlighting the proven advantages of hearing aids, which can bring improvements in the user’s social, psychological and physical sense of wellbeing.
Specific benefits include:
- Greater ease in hearing and following conversations – aiding sociability and improved interaction with friends and family
- Greater ease of enjoyment of television and radio
- Reduced impact and disturbance from tinnitus.
Findings from a recent study provide further impetus to try hearing aids. The study, which included 3,777 participants aged 65 years and over, showed that hearing loss was linked to an increased risk of both disability and dementia (as well as depression in men).6 This higher risk was not seen in people who used hearing aids.
Commenting on the findings, Dr Clare Walton, research manager at the Alzheimer’s Society, notes: “By following people over 65 years of age, with and without hearing problems for up to 25 years, researchers found that those with hearing problems were more likely to develop dementia. Although this type of study cannot tell us whether using hearing aids would help to bring the risk of dementia back down, it does hint that this might be the case.”7
For those concerned about the ‘optics’ of hearing aids, pharmacy staff should explain that most modern devices are small, discrete and comfortable to wear. It is also important to signpost customers to additional sources of support such as the charity Action on Hearing Loss, which provides a comprehensive step-by-step guide to help patients adjust to life with a hearing aid.
Research shows that it takes around a month to acclimatise to hearing aids and obtain maximum benefit from their use – so customers should be encouraged to persevere.
Cochlear implants
Cochlear implants are hearing implants usually reserved for those children with severe to profound permanent deafness who have derived limited or no benefit from hearing aids. They consist of an internal receiver that is surgically implanted under the skin behind the ear and an external component known as a speech processor, which is similar to a hearing aid and includes the microphone.
It is generally recommended that implants are fitted at a young age (usually before one year) to maximise potential benefits.
References
- Action on Hearing Loss
- The Mental Health Foundation: Earwax
- NICE Clinical Knowledge Summaries (CKS). Otitis externa. Updated February 2018
- BUPA
- NICE Clinical Knowledge Summaries (CKS). Otitis media: acute. Updated July 2018
- Amieva H et al. Death, depression, disability and dementia associated with self-reported hearing problems: a 25-year study.
The Journals of Gerontology 2018; 73(10): 1383-1389 - Alzheimer’s Society: Study confirms the link between hearing loss and dementia in older adults.
