Beyond the surface
In OTC
Follow this topic
Bookmark
Record learning outcomes
Skin conditions are often only regarded as a physical problem, but the psychological impact can create issues that go much deeper
Having a skin condition such as acne or psoriasis can negatively impact people way below the surface of the skin. In fact, nine out of 10 dermatologists agree that not enough importance is placed on the psychological effects resulting from skin conditions, according to a survey by the British Skin Foundation (BSF).

Each year, 54 per cent of the population is affected by skin disease, according to The Crisis in Dermatology report, published in the British Medical Journal in 2015. Acne, rosacea, eczema and psoriasis are just some of the skin conditions that can incite mental health issues such as anxiety, depression and even skin disease-specific issues such as acne excoriée (see below).
“As issues with the skin are so outwardly visible to others, it is not surprising that those who suffer may also feel embarrassment and psychological distress in addition to potential physical pain that skin conditions like eczema and acne can cause. They may avoid participating in social activities or wearing clothing that expose affected areas; such withdrawal in behaviour can reinforce, and thereby exacerbate, the low self-confidence,” says Dr Anjali Mahto, consultant dermatologist and BSF spokesperson.
“Additionally, the symptoms of skin disease, which can be severe, are often underestimated by those not directly affected. The preoccupation society and social media have with self-image, and their stigmatisation of perceived imperfections, only creates further pressure,” she adds.
Dr Bav Shergill, consultant dermatologist and spokesperson for the British Association of Dermatologists explains that there can also be a vicious cycle involved. “It’s not uncommon for dermatology patients to experience social anxiety, depression and appearance-related distress and stress is commonly an issue with skin disease patients. As well as being potentially triggered by their condition, [stress] can also be something that causes their skin to flare up. Not only does our skin have an impact on our mental health, but our mental health can have an impact on our skin health,” he says.
Support to shout about
The psychological impact of skin conditions varies from person to person, as does the support that they need. However, according to the BSF, 87 per cent of dermatologists say that people with skin conditions in the UK do not have sufficient access to psychological support for these issues.
“The effects of skin disease on mental health has only been recognised over the last few decades, but we are now seeing a change in attitudes as it is becoming accepted as a real issue,” explains Dr Mahto. “Unfortunately, in some areas, there may not be as much support for people with skin conditions – such as access to psychiatrists and psychologists – as we would like. This is likely due to limited resources and funding on the NHS.”
However, there is support available in a variety of different guises and pharmacy teams can help make customers aware of their options and how to go about seeking support.
“There is a wide range of techniques and self care techniques out there, but it depends on the needs of the patient. The most important thing pharmacists can do is raise awareness amongst people that if they are struggling with their mental health because of their condition they should be raising this with their GP or dermatologist, and they should consider some of the self-help materials that are available. These can include cognitive behavioural therapy, habit reversal, or advice on developing self-confidence in social environments,” says Dr Shergill.
Dr Mahto agrees, explaining “if someone is suffering with their skin and it is affecting daily activities, causing problems with low mood, poor self-esteem, anxiety or depression it is vital to seek medical help.” She adds that pharmacy teams can also signpost customers to local therapy groups, online support groups and forums, even if they aren’t skin-specific.
54 per cent of the population is affected by skin disease
Specific skin support
The Sheffield Improving Access to Psychological Therapies (IAPT) service for living well with skin conditions specifically focuses on providing self-help resources and guides for people living with skin conditions. This includes a five-week course entitled ‘Living well with a skin condition’, which involves weekly wellbeing sessions lasting 2.5 hours. The course aims to find ways of managing the physical symptoms of skin conditions and the impact these symptoms have on mood, learning how to manage low mood stress and anxiety and dealing with worries about skin conditions.
Pharmacy teams based in the city can signpost customers to more information here.
Psychodermatology explained
The British Association of Dermatologists (BAD) is dedicated to providing psychological support for people with skin diseases using psychodermatology – the treatment of skin issues with psychological methods. Treatment can be tailored to an individual and should help to relieve stress, anxiety and depression, which can all worsen skin problems. Treatment focus can include:
- Reversing beliefs about appearance and attractiveness
- Understanding the relationship between stress and skin disorder
- Learning how to cope with a skin problem
- Stopping bad habits such as itching
- Building self-esteem
- Building relationships
- Building social interaction skills
- Managing psychological distress.
According to BAD, studies have shown that amongst people who completed psychodermatology therapies, 94 per cent reported reduced stress and 92 per cent reported increased confidence. Because this is still a developing area, customers may not be aware this support exists, so pharmacy teams can make customers aware of psychodermatology services and the referral processes in their area.
All about acne
An estimated 80 per cent of people aged 11 to 30 have acne outbreaks at some point, according to the National Institute of Arthritis and Musculoskeletal and Skin Diseases.
For people prone to acne, it occurs when there is a build-up of oil on the skin, blocking pores and causing the bacteria propionibacterium acnes to multiply. This triggers the formation of tender, pus-filled spots, blackheads and whiteheads, which can make the skin feel painful and hot. Acne commonly appears on the face but can also appear across the neck, chest and back.
People with acne can often feel self-conscious and anxious in social situations and there are other psychological conditions that can occur as a result, such as:
- Acne dysmorphic disorder (ADD) is when a person is consumed by negative thoughts about how bad their acne is. This can lead to low mood and depression and have a negative impact on a person’s self worth
- Acne excoriée, also known as pickers acne, causes people to pick or squeeze acne lesions, which often leads to scabs and scarring. According to BAD’s Acne Support website, it is not uncommon for someone with this condition to pick out every acne lesion on their body. The condition is thought to be associated with underlying depression, anxiety and emotional problems and is most often seen in teenage girls.
For the physical treatment of acne, pharmacy teams can recommend an over-the-counter (OTC) cream or gel containing benzoyl peroxide, salicylic acid or nicotinamide. If necessary, customers can get stronger treatments on prescription, such as isotretinoin. But perhaps most importantly, pharmacy teams can let customers with acne know that there is mental health support available too. Acne Support has a whole host of helplines and advice available based on the specific mental impact of acne, at: acnesupport.org.uk.
The effects of skin disease on mental health has only been recognised over the last few decades
Recognising rosacea
Rosacea is thought to affect one in 10 people. It mainly appears on the face and is more common in women than men. Symptoms include redness on the chin, cheeks, nose and forehead that can have a burning or stinging sensation when cleaning the face. Other symptoms can include dry skin, red spots, swelling, sore eyelids, yellow-orange patches and thickened skin, especially on the nose.
The cause of rosacea is unknown but it can be triggered by alcohol, caffeine, hot drinks, spicy food, cheese and even aerobic exercise. The condition cannot be cured but it can be controlled with prescription creams and a course of topical antibiotics such as metronidazole. Pharmacy teams can also advise customers to wear high SPF sun cream, avoid heat and sunlight, clean their eyelids regularly and use gentle facial products. As with other skin conditions, stress management is also a key part of controlling rosacea.
The National Rosacea Society has a page dedicated to helping people manage uncomfortable questions about the condition.
Explaining eczema
In the UK, one in five children and one in 12 adults have eczema, while eczema and contact dermatitis account for 84-90 per cent of skin disease related to hazards at work, according to the National Eczema Society.
In addition, a survey by Allergy UK in 2017 found that over 70 per cent of people with eczema reported feeling depressed as a result of their eczema and one in 10 consumed more alcohol when their eczema was at its worst.
Also known as dermatitis, eczema is a dry skin condition that varies from person to person. The skin is itchy, scaly and dry in mild cases and in more severe cases can appear to weep, form a crust and bleed. Because the condition can be both painful and itchy, scratching often occurs leaving the damaged skin and susceptible to infection.
Believed to be a genetic condition, eczema is also triggered by environmental factors and can occur if the skin fails to produce enough oil and fat. This means the skin is unable to form a protective barrier, making it more vulnerable to infection, itching and inflammation.
There is no cure for eczema but it can be managed with emollients, which should be used daily to moisturise the skin and prevent it becoming dry. Another option includes topical corticosteroids, which can reduce swelling and redness. Pharmacy teams can also advise customers to avoid scratching sore spots and keep nails short if customers are finding it too hard to stop scratching.
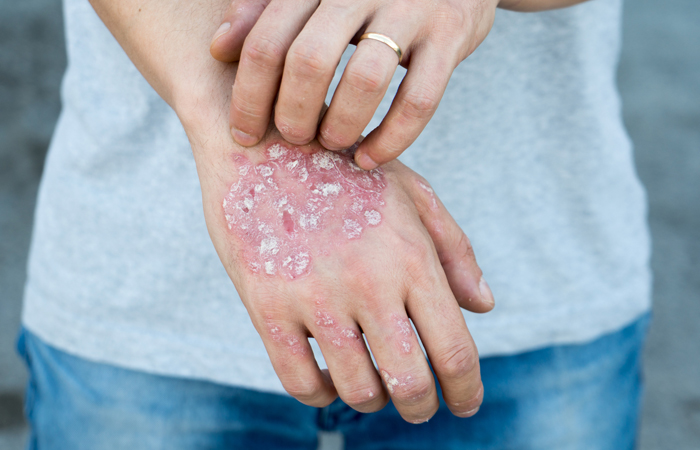
Soothing psoriasis
Up to 1.8 million people in the UK have psoriasis, according to the Psoriasis Association. In a collaborative report, See psoriasis: look deeper, by the Mental Health Foundation and the Psoriasis Association, some 77 per cent of people affected by psoriasis describe it as a problem or significant problem impacting their quality of life and approximately one third of people experience depression and anxiety with the condition.
Psoriasis can appear anywhere on the body but it often appears on the scalp, knees and elbows as red, flaky, crusty patches of skin identified by silvery scales. It is not known exactly what causes the condition, but it has previously been linked to issues with the immune system. There is no cure for psoriasis but there are topical treatments that can manage the condition.
Like eczema, daily use of emollients can keep the skin hydrated. Specialist treatments such as phototherapy (light treatment), vitamin A and D tablets and topical steroids can be prescribed by a GP and dermatologist.
Guided mindfulness and meditation to help people with psoriasis manage stress, anxiety and depression can be found via the BAD’s Skin Support website.
Acne answers
Curtis Williams, who is now 24, suffered with acne from the age of 13. After using a variety of drugs and creams bought over the counter and on prescription, he went on a three-month treatment course of the isotretinoin known as Roaccutane. After three months the acne spots were mostly gone but it took another four to five months for the redness and swelling to completely disappear. Now Curtis has clear skin and no acne scars. He talks to TM about his experiences
Did having acne make you think about how people saw you?
“I was definitely conscious of my acne when talking to or meeting people. I felt like I wasn’t good looking at the time. And I do think people maybe looked at me differently when my acne cleared up after Roaccutane, which I guess came as a confidence boost once it had gone.”
Did you feel like there was anywhere to get mental health support for your skin condition?
“No, not really. The only time my mental health was checked in on was when I was receiving Roaccutane treatment, because one of the side effects was increased risk of suicide. So doctors regularly checked in during that treatment, and my parents were advised to check on my mental health. But apart from that, no.”
How much did you think about your skin when you had acne?
“It was impossible not to think about it multiple times a day, mainly as mine was pretty painful and I could physically feel it. And anytime I caught myself in the mirror I would check to see if the spots had got worse or better. So it was always there. Imagine when you have a big spot on your face, you check it regularly during the day whilst at work or school. Now imagine you have 25 of those all over your face and they’re red and swollen. It’s impossible not to think about it.”
How did you find out about treatment?
“I was very lucky to have my mum as a support network when I was really suffering from it, because she had experienced it herself and had to push really hard through the NHS to go from the low level drugs like oxytetracycline to the harsher treatment of Roaccutane. And she did exactly the same for me, I wouldn’t have even known about it. The GPs don’t really make you aware of it unless you push for it. I was lucky it cleared up when I was young, because I do think if I was going to university with the acne then it really would have started to affect me mentally. I think my confidence would have been really bad.”
While Roaccutane might not be suitable for all customers, Curtis’s story proves that encouraging people suffering with acne to discuss all their options with the GP can make a huge difference to their physical and mental health.
